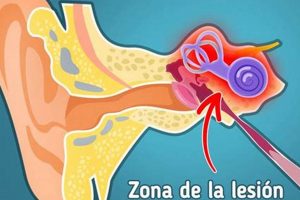
The sensation of ringing, buzzing, or hissing noises in the ear, often described as tinnitus, is a common auditory experience. The perception of these sounds occurs without an external source and can vary significantly in intensity and frequency. The experience can be intermittent or constant, and it may manifest in one or both ears.
Understanding the potential causes of this auditory perception is crucial for appropriate management and treatment. Contributing factors can include exposure to loud noises, age-related hearing loss, ear infections, and certain medical conditions, such as Meniere’s disease. In some instances, specific medications or head injuries can also trigger or exacerbate the condition. Addressing the underlying cause is often essential for alleviating the discomfort.
The subsequent sections will delve into the various potential etiologies of perceived ear ringing, diagnostic approaches employed to identify the root cause, and available treatment options designed to mitigate the symptoms and improve the individual’s overall quality of life. This exploration aims to provide a comprehensive overview of this auditory phenomenon and guide readers toward appropriate care and management strategies.
Addressing Persistent Ear Ringing
Individuals experiencing persistent ear ringing, often medically referred to as tinnitus, should consider the following guidelines to potentially mitigate the condition and improve their overall well-being. Implementing these suggestions does not guarantee a cure, but may assist in managing the symptoms.
Tip 1: Reduce Exposure to Loud Noises: Minimize time spent in environments with high noise levels. When unavoidable, utilize appropriate hearing protection, such as earplugs or earmuffs.
Tip 2: Manage Stress Levels: Practice relaxation techniques like deep breathing exercises, meditation, or yoga. Stress can exacerbate the perception of tinnitus.
Tip 3: Limit Caffeine and Alcohol Consumption: These substances can stimulate the nervous system and potentially worsen tinnitus symptoms. Monitor intake and consider reducing consumption.
Tip 4: Ensure Adequate Sleep: Establish a regular sleep schedule and create a conducive sleep environment. Sleep deprivation can contribute to increased tinnitus perception.
Tip 5: Monitor Blood Pressure: High blood pressure can contribute to tinnitus. Maintain regular blood pressure checks and follow medical advice for management.
Tip 6: Review Medications: Certain medications can have tinnitus as a side effect. Consult a physician to review current medications and explore potential alternatives if applicable.
Tip 7: Consider White Noise Therapy: Utilize white noise machines, fans, or nature sounds to mask the tinnitus sound and make it less noticeable, especially during quiet periods like bedtime.
By consistently implementing these strategies, individuals experiencing persistent ear ringing may find some relief from their symptoms. It is crucial to understand that the effectiveness of these tips can vary significantly from person to person.
The subsequent section will focus on when to seek professional medical attention for tinnitus and what diagnostic procedures may be involved in determining the underlying cause. This aims to provide further guidance on managing and addressing this condition effectively.
1. Noise exposure duration
The duration of exposure to elevated sound pressure levels directly influences the likelihood and severity of tinnitus, characterized by a persistent ringing or buzzing in the ears. Prolonged exposure to loud noises, particularly without adequate hearing protection, initiates a cascade of physiological effects within the auditory system. Specifically, intense sound waves cause damage to the delicate hair cells located in the inner ear, responsible for transducing sound vibrations into electrical signals for the brain to interpret. This cellular damage can result in temporary or permanent hearing loss, alongside the perception of tinnitus.
The correlation between noise exposure duration and tinnitus severity is not always linear; however, longer exposure times generally correlate with a higher risk of permanent auditory damage. For instance, individuals working in industrial settings with continuous machinery noise or those frequently attending loud music concerts without hearing protection are at a significantly increased risk. This effect is compounded by the cumulative nature of auditory damage, meaning that even seemingly minor exposures over extended periods can contribute to the eventual onset of tinnitus. Proper use of hearing protection devices, such as earplugs or earmuffs, is critical in mitigating the harmful effects of prolonged noise exposure. Furthermore, regular audiometric testing can help monitor an individual’s hearing health and detect early signs of noise-induced hearing loss or tinnitus.
In summary, the duration of noise exposure constitutes a primary factor in the development and severity of tinnitus. Understanding this relationship is crucial for implementing preventative measures, particularly in occupational and recreational settings characterized by high noise levels. Consistent and proper use of hearing protection, coupled with regular hearing evaluations, offers the most effective strategy for minimizing the risk of noise-induced auditory damage and the subsequent manifestation of tinnitus.
2. Underlying medical conditions
Various medical conditions can manifest as, or contribute to, the perception of ear ringing, often described as tinnitus. The presence of specific underlying health issues may directly impact the auditory system or indirectly influence neurological pathways involved in sound processing, thereby triggering or exacerbating tinnitus symptoms. Identifying and addressing these underlying conditions is often crucial for effective tinnitus management.
- Cardiovascular Disorders
Conditions such as hypertension (high blood pressure), atherosclerosis (hardening of the arteries), and other cardiovascular ailments can affect blood flow to the inner ear, potentially disrupting its function and leading to tinnitus. Altered blood flow patterns can cause turbulent or pulsatile tinnitus, where individuals perceive a rhythmic throbbing or whooshing sound in sync with their heartbeat. Managing cardiovascular health through medication, lifestyle changes, and dietary adjustments is essential for mitigating this type of tinnitus.
- Neurological Conditions
Neurological disorders, including multiple sclerosis, head injuries, and acoustic neuromas (benign tumors on the auditory nerve), can disrupt the normal processing of auditory signals in the brain, resulting in tinnitus. These conditions may affect the neural pathways responsible for sound perception, leading to abnormal activity and the subjective experience of phantom sounds. The management of neurologically-related tinnitus often requires specialized medical interventions and therapies.
- Metabolic Disorders
Metabolic conditions, such as diabetes, thyroid disorders, and vitamin deficiencies, can indirectly contribute to tinnitus by affecting nerve function and overall health. For instance, uncontrolled diabetes can damage small blood vessels and nerves throughout the body, including those in the inner ear. Similarly, thyroid imbalances can disrupt metabolic processes that are crucial for auditory nerve function. Addressing these metabolic imbalances through medication and lifestyle changes can help alleviate tinnitus symptoms.
- Meniere’s Disease
Meniere’s disease is a disorder of the inner ear characterized by episodes of vertigo (dizziness), hearing loss, tinnitus, and a feeling of fullness in the ear. This condition is thought to be caused by an abnormal buildup of fluid in the inner ear, which disrupts its normal function. Tinnitus associated with Meniere’s disease can be particularly distressing and may require specific medical interventions, such as medication or surgery, to manage the symptoms.
These examples illustrate the complex interplay between underlying medical conditions and the perception of ear ringing. A thorough medical evaluation is essential for identifying any contributing health issues and developing an appropriate treatment plan. Addressing these underlying conditions can significantly improve tinnitus management and the individual’s overall quality of life.
3. Medication side effects
Certain medications possess the potential to induce or exacerbate tinnitus, the perception of ringing or buzzing in the ears. This phenomenon arises as a result of the ototoxic properties inherent in some pharmaceutical compounds, directly affecting the delicate structures within the inner ear responsible for auditory transduction. The degree to which a medication contributes to tinnitus varies, contingent upon factors such as dosage, duration of use, and individual susceptibility. Examples of pharmaceuticals associated with ototoxicity include certain antibiotics (aminoglycosides), anti-inflammatory drugs (high doses of aspirin), chemotherapy agents (cisplatin), and loop diuretics (furosemide). The mechanism of action often involves damage to the cochlear hair cells, which are critical for sound reception.
The importance of recognizing medication-induced tinnitus lies in the possibility of intervention. Upon identification of a potential causative agent, consultation with a healthcare professional is warranted to evaluate the feasibility of alternative therapies or dosage adjustments. In some cases, cessation of the offending medication may lead to a reduction or elimination of tinnitus symptoms, though the reversibility of ototoxic damage is not always guaranteed. Furthermore, proactive monitoring for auditory changes during treatment with known ototoxic drugs is crucial for early detection and management.
In summary, medication side effects represent a significant etiological factor in the manifestation of tinnitus. Recognizing the potential for drug-induced auditory changes and implementing appropriate monitoring and management strategies are essential for mitigating the adverse effects of medication on hearing health. A thorough review of a patient’s medication history is a critical component of any evaluation of persistent ear ringing, facilitating informed decisions regarding treatment and prevention.
4. Hearing loss presence
The presence of hearing loss is frequently associated with the perception of tinnitus, the sensation of ear ringing or buzzing, often expressed as “por qu me zumba mucho el odo.” This connection arises from the brain’s attempt to compensate for diminished auditory input. When the ear’s ability to transmit sound signals decreases, the brain may increase neural activity in auditory pathways to heighten sensitivity. This heightened activity can be misinterpreted as sound, leading to the subjective experience of tinnitus. The degree of hearing loss does not always correlate directly with the intensity of tinnitus; even mild hearing loss can trigger significant ringing.
The correlation between hearing loss and tinnitus has practical implications for diagnosis and management. Audiological evaluations are crucial for individuals experiencing persistent ear ringing to identify any underlying hearing impairment. Addressing the hearing loss through amplification devices, such as hearing aids, can often reduce the perceived tinnitus by restoring a more normal auditory input to the brain. In cases where hearing loss is not directly treatable, other tinnitus management strategies, such as sound therapy or cognitive behavioral therapy, may be employed to help individuals cope with the condition. Real-life examples include individuals with age-related hearing loss who develop tinnitus and find relief through the use of hearing aids.
Understanding the relationship between hearing loss and tinnitus is essential for effective clinical intervention. Identifying and managing hearing loss can be a critical step in alleviating the distress associated with tinnitus and improving an individual’s overall quality of life. While not all instances of tinnitus are directly related to hearing loss, its presence significantly increases the likelihood of experiencing this auditory phenomenon. Comprehensive audiological assessments and personalized management plans are therefore paramount in addressing this complex issue.
5. Stress and anxiety
Stress and anxiety function as significant exacerbating factors in the experience of tinnitus. While not typically considered direct causal agents, heightened states of psychological distress frequently amplify the perception of ear ringing or buzzing. The physiological mechanisms underlying this connection involve the activation of the sympathetic nervous system, leading to increased muscle tension, elevated blood pressure, and heightened sensitivity to sensory stimuli. These physiological changes can amplify the auditory processing of the internal sounds associated with tinnitus, making them more pronounced and bothersome.
The interaction between stress and tinnitus operates in a cyclical manner. The presence of tinnitus itself can be a source of considerable stress and anxiety, creating a feedback loop that perpetuates and intensifies both the tinnitus symptoms and the emotional distress. Individuals experiencing chronic stress or anxiety disorders may be particularly vulnerable to this cycle. For example, a high-pressure work environment or ongoing personal challenges can contribute to heightened anxiety levels, which in turn amplify the awareness and intensity of tinnitus. This can lead to a decrease in overall quality of life, impacting sleep, concentration, and emotional well-being. Real-world scenarios frequently demonstrate that periods of increased stress, such as during exam times for students or during periods of intense professional deadlines, are associated with a noticeable worsening of tinnitus symptoms.
Effective management of tinnitus therefore necessitates a holistic approach that addresses both the auditory perception and the underlying psychological factors. Stress reduction techniques, such as mindfulness meditation, deep breathing exercises, and cognitive behavioral therapy, can play a crucial role in breaking the cycle between stress and tinnitus. By learning to manage and reduce anxiety levels, individuals can decrease their focus on the internal sounds and improve their ability to cope with the condition. This integrated approach highlights the importance of recognizing and addressing psychological well-being as an integral component of comprehensive tinnitus care.
6. Caffeine/alcohol intake
The consumption of caffeine and alcohol can significantly influence the experience of tinnitus, often characterized by persistent ear ringing or buzzing. These substances exert their effects on the auditory system through various physiological mechanisms. Caffeine, a stimulant, increases neural activity and blood pressure, which may amplify existing tinnitus or trigger its onset in susceptible individuals. Alcohol, while initially possessing depressant qualities, can disrupt inner ear fluid balance and alter auditory nerve function, potentially exacerbating tinnitus symptoms. The precise mechanisms are complex and vary among individuals.
The role of caffeine and alcohol intake as components contributing to tinnitus lies in their ability to modulate neural excitability and vascular dynamics within the auditory system. For example, excessive caffeine consumption can lead to heightened sensory perception, making the perceived ringing sound more noticeable. Conversely, alcohol-induced vasodilation and subsequent fluid retention may affect the delicate structures of the inner ear, disrupting auditory signal processing. Observational evidence supports these associations, with numerous individuals reporting increased tinnitus severity following consumption of caffeinated beverages or alcoholic drinks. The sensitivity to these substances can vary considerably; some individuals may experience a marked increase in tinnitus symptoms, while others may notice little to no change.
Understanding the connection between caffeine/alcohol intake and tinnitus is of practical significance for managing the condition. Individuals experiencing persistent ear ringing are often advised to monitor their consumption of these substances and to experiment with reducing or eliminating them from their diet to assess any impact on their tinnitus symptoms. While this approach may not eliminate tinnitus entirely, it can often provide a degree of relief and improve overall quality of life. The challenge lies in identifying individual sensitivities and establishing personalized dietary modifications based on empirical observation and professional guidance. Furthermore, the effects of caffeine and alcohol can be compounded by other lifestyle factors, such as stress, sleep deprivation, and noise exposure, highlighting the need for a comprehensive approach to tinnitus management.
7. Earwax blockage
Earwax blockage, or cerumen impaction, can contribute to the sensation of ear ringing, often described as “por qu me zumba mucho el odo.” The accumulation of earwax within the ear canal can physically obstruct the transmission of sound waves to the inner ear, leading to altered auditory perception. This blockage can create pressure on the eardrum and disrupt the normal mechanics of hearing. The altered pressure and compromised sound transmission can manifest as tinnitus, presenting as a ringing, buzzing, or muffled sound in the affected ear. The degree to which earwax blockage induces tinnitus varies, contingent upon the extent of the impaction and individual sensitivity. For example, an individual with pre-existing mild hearing loss may experience a more pronounced tinnitus sensation due to the added blockage exacerbating their underlying auditory condition.
The practical significance of understanding this connection lies in the relative ease with which earwax blockage can be diagnosed and treated. A simple otoscopic examination by a healthcare professional can readily identify the presence of cerumen impaction. Removal of the obstructing earwax, typically through irrigation, manual removal, or cerumenolytic agents, often resolves the associated tinnitus. Real-life examples include individuals who experience sudden onset of ear ringing following activities that may push earwax deeper into the ear canal, such as using cotton swabs. Upon professional removal of the impacted earwax, the tinnitus subsides, restoring normal auditory function. It’s important to note that attempting self-removal of earwax can be counterproductive and may further exacerbate the impaction or damage the ear canal.
In summary, earwax blockage represents a potentially reversible cause of tinnitus. While other, more complex etiologies of ear ringing exist, assessing for and addressing cerumen impaction is a crucial first step in the diagnostic process. Timely and appropriate management of earwax blockage can alleviate the bothersome symptoms of tinnitus and prevent further complications, contributing to improved auditory health and overall well-being. The uncomplicated nature of this intervention underscores the importance of considering earwax blockage as a potential factor when individuals present with complaints of persistent ear ringing.
Frequently Asked Questions
This section addresses common inquiries regarding the experience of persistent ear ringing, providing concise and informative answers to enhance understanding of this auditory phenomenon.
Question 1: What are the primary causes of persistent ear ringing?
Common causes include noise exposure, age-related hearing loss, ear infections, Meniere’s disease, certain medications, and head injuries. Underlying medical conditions such as cardiovascular disorders and neurological issues can also contribute.
Question 2: Is persistent ear ringing a sign of a serious medical condition?
While not always indicative of a serious underlying issue, persistent ear ringing can sometimes signal an underlying medical condition. It is advisable to seek professional medical evaluation to determine the cause and rule out any serious health concerns.
Question 3: Can persistent ear ringing be cured completely?
A definitive cure is not always possible, particularly when caused by permanent damage such as noise-induced hearing loss. Management strategies focusing on symptom reduction and improving coping mechanisms are often employed.
Question 4: What are effective strategies for managing the symptoms of persistent ear ringing?
Effective strategies include reducing noise exposure, managing stress, limiting caffeine and alcohol consumption, ensuring adequate sleep, monitoring blood pressure, reviewing medications with a physician, and considering white noise therapy.
Question 5: When should a medical professional be consulted about persistent ear ringing?
Medical consultation is advisable when the ringing is persistent, severe, accompanied by other symptoms such as hearing loss or dizziness, or significantly impacts daily life. A medical professional can conduct necessary evaluations to determine the cause and recommend appropriate management strategies.
Question 6: Can earwax blockage cause ear ringing, and is it easily treatable?
Yes, earwax blockage can contribute to ear ringing. It is typically a reversible cause and can be effectively treated through professional earwax removal, often resolving the associated tinnitus.
Understanding the multifaceted nature of persistent ear ringing and exploring appropriate management strategies are essential for enhancing individual well-being. The information presented herein is for informational purposes and does not substitute professional medical advice.
The subsequent section will delve into various therapeutic modalities that are designed to address ear ringing and alleviate symptoms.
Understanding the Experience of Persistent Ear Ringing
This exploration has elucidated the multifaceted factors contributing to the perception of persistent ear ringing. The analysis encompassed diverse etiologies, ranging from auditory damage resulting from noise exposure and medical conditions such as Meniere’s disease, to lifestyle elements including caffeine and alcohol consumption and even the simple presence of earwax blockage. The significant role of psychological factors, particularly stress and anxiety, in exacerbating the subjective experience was also emphasized. The necessity of identifying underlying causes, when possible, to direct appropriate management strategies has been a recurring theme.
The phenomenon of “por qu me zumba mucho el odo” warrants serious consideration and responsible action. Seeking professional medical evaluation is paramount for individuals experiencing persistent ear ringing, to determine the underlying cause and implement a comprehensive management plan. While a definitive cure may not always be attainable, proactive intervention can significantly improve an individual’s quality of life and mitigate the disruptive impact of this auditory condition. Continued research and development of new therapeutic modalities remain essential for advancing the understanding and treatment of tinnitus.